Scientific
newsletters

A precise description of the clinical subtypes of multiple sclerosis is necessary in order to better classify each patient’s disease and better tailor their immunomodulatory therapy according to its course. The earlier classification of 1996 has been reviewed in 2013 and published in 2014 by Fred Lublin and co-workers.
The current classification of disease courses
The radiologically isolated syndrome.
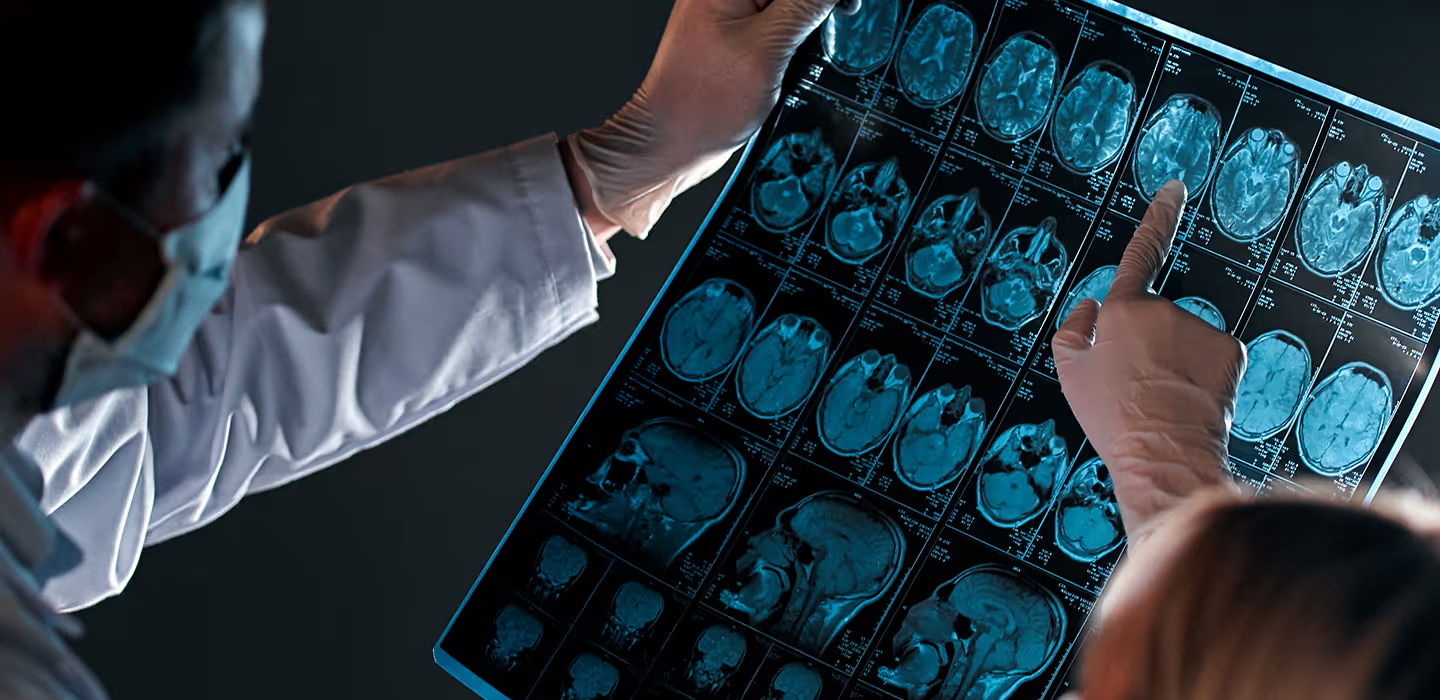
This consists in the incidental discovery of lesions highly suspected of being multiple sclerosis plaques but detected by brain magnetic resonance imaging (MRI) performed for any other reason, such as a headache, cranial trauma, a suspected pituitary tumour, etc. It involves patients who have never shown any symptoms of multiple sclerosis but who could potentially develop the disease later on.
The clinically isolated syndrome.
This refers to persons experiencing a first inflammatory event in the central nervous system, displaying symptoms typical of multiple sclerosis. There is, however, no dissemination of lesions, either in the central nervous system (only a single lesion is detectable), or over time (there are no inactive previous lesions, and only one new active lesion). In the absence of such a dissemination in space and time, a multiple sclerosis diagnosis cannot be made.
Relapsing-remitting multiple sclerosis.
This is the predominant form of multiple sclerosis (55%), with exacerbations (“relapses”) varying in frequency and intensity. It can either be followed by a complete recovery or can leave permanent damage, but shows no worsening of symptoms between exacerbations. The symptoms appear and worsen in a few hours or in a few days and must persist for more than 24 hours without fever. This form of multiple sclerosis can be inactive, either spontaneously or thanks to immunomodulatory therapies, or active, if clinical exacerbations occur and/or if MRI shows new lesions when compared to previous imaging.
Progressive multiple sclerosis.
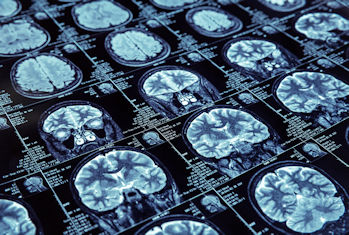
This consists of a progressive increase of neurological deficits over the course of several months, either at the onset of the disease, without any initial exacerbation (primary-progressive type), or after a first phase of exacerbations and remissions (secondary-progressive type). At this time, we do not yet have specific and precise criteria to determine the moment of transition from the relapsing-remitting type to a secondary-progressive type. This progression must be evaluated at least once a year using the “EDSS” disability scale and must be differentiated from the accumulation of deficits due to previous exacerbations.
We can distinguish four subtypes for both the primary and secondary progressive types:
Active with progression
Active without progression
Inactive with progression
Inactive without progression (in this case, the disease is stabilised at a “plateau” which remains susceptible to changing later).
The term “active” denotes the presence of exacerbations in addition to a progression and/or a change in the MRI. The term “progression” means the aggravation of symptoms over a period of several months, as measured by the EDSS scale.
The fact that the severity and activity of the disease can change significantly but unpredictably throughout its course must be emphasized. The term “benign”, with regard to MS, always refers to a retrospective diagnosis which can only be given after a disease’duration of 20 to 30 years.
It is therefore up to each patient and his/her neurologist to regularly determine, together and at least once a year, the course and characteristics of his/her disease.
Prof. Dr. Christian Sindic

Newsletter 44
Stay informed
Receive all the information related to research and news from the Belgian Charcot Foundation directly in your inbox.